|

There is a lot of to know about
Parkinson's
disease. You may be wondering what it is, how it is
diagnosed, and what treatment options are available. The
National Parkinson Foundation is here to help you navigate
through all of your questions and concerns. Get started now.
What is Parkinson’s
disease?
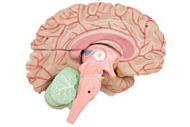 Parkinson’s
disease (PD) is a
neurodegenerative brain disorder that progresses slowly
in most people. What this means is that individuals with PD will
be living with PD for twenty years or more from the time of
diagnosis. While Parkinson’s disease itself is not fatal, the
Center for Disease Control rated complications from the disease
as the 14th top cause of death in the United States. There is
currently no cure for Parkinson’s; however, your doctors will be
focused and dedicated to finding treatments that help control
the symptoms of PD and have a good quality of life. Parkinson’s
disease (PD) is a
neurodegenerative brain disorder that progresses slowly
in most people. What this means is that individuals with PD will
be living with PD for twenty years or more from the time of
diagnosis. While Parkinson’s disease itself is not fatal, the
Center for Disease Control rated complications from the disease
as the 14th top cause of death in the United States. There is
currently no cure for Parkinson’s; however, your doctors will be
focused and dedicated to finding treatments that help control
the symptoms of PD and have a good quality of life.
Normally, there are brain
cells (neurons) in the human brain that produce
dopamine.
These neurons concentrate in a particular area of the brain,
called the
substantia nigra. Dopamine is a chemical that relays
messages between the substantia nigra and other parts of the
brain to control movements of the human body. Dopamine helps
humans to have smooth coordinated muscle movements. When
approximately 60 to 80% of the dopamine-producing cells are
damaged, and do not produce enough dopamine, the motor symptoms
of Parkinson’s disease appear. This process of impairment of
brain cells is called neurodegeneration.
The current theory (so-called Braak’s hypothesis) is that the
earliest signs of Parkinson’s are found in the enteric nervous
system, the medulla and in particular, the olfactory bulb, which
controls your sense of smell. Under this theory, Parkinson’s
only progresses to the substantia nigra and cortex over the
years. This theory is increasingly borne out by evidence that
non-motor symptoms, such as a loss of sense of smell, hyposmia,
sleep disorders and constipation may precede the motor features
of the disease by several years. For this reason, researchers
are increasingly focused on these “non-motor” symptoms to both
detect PD as early as possible and to look for ways to stop its
progression.
What are the symptoms of Parkinson's
disease?

Four Main Motor Symptoms of PD:
- Shaking or
tremor
at rest.
- Slowness of movement, called
bradykinesia.
- Stiffness or
rigidity of the arms, legs or
trunk.
- Trouble with balance and falls, also called
postural instability. Postural instability usually
appears later with disease progression and may not be
present with initial diagnosis.
Secondary Symptoms of PD May Include:
- Small, cramped handwriting, called
micrographia.
- Reduced arm swing on the affected side.
- Slight foot drag on affected side creating a shuffled
walk.
- “Freezing”—a
term used to describe the phenomenon of being “stuck in
place” when attempting to walk.
- Loss of facial expression due to rigidity of facial
muscles, called
hypomimia.
- Low voice volume or muffled speech, called
hypophonia.
- Tendency to fall backwards, called
retropulsion.
- Decrease ability in automatic reflexes such as
blinking and swallowing.
Other Symptoms of PD
-
Depression
-
Anxiety- beyond the normal response to stress
-
Hallucinations,
psychosis
- Sleep disturbances (vivid dreams, talking and moving
during night sleep)
- Constipation
- Pain
- Increase in dandruff (seaborrhea dermatitis) or oily
skin
Table 1. Symptoms in Parkinson’s disease
| MOTOR SYMPTOMS |
| Bradykinesia (slowness of movement) |
| Rigidity (stiffness of movement) |
| Tremor (involuntary shaking of the hands, feet,
arms, legs, jaw, or tongue, usually more prominent at
rest) |
| Postural Instability (tendency to fall without
explanation, usually when pivoting) |
| NON-MOTOR SYMPTOMS |
| Mood (depression, anxiety, irritability) |
| Cognitive changes (attention, visuo-spatial
problems, memory problems, personality changes,
psychosis/hallucinations) |
| Orthostatic hypotension (lightheaded and low blood
pressure upon standing) |
| Constipation and early satiety (a feeling of
fullness after eating small amounts) |
| Hyperhidrosis (excessive sweating), especially of
hands and feet |
| Seborrhea dermatitis (dry skin) dandruff |
| Urinary urgency, frequency and incontinence |
| Loss of sense of smell (Anosmia) |
| Sleep disorders |
| Insomnia, Excessive Daytime Sleepiness (EDS), Rapid
Eye Movement Behavioral Disorder (RBD) or active
dreaming, dream enactment, involuntary movements and
vocalizations during sleep, Restless Legs Syndrome (RLS)/Periodic
Leg Movements Disorder (PLMD) |
| Sensory (pain, tightness, tingling, burning) |
| MIXED MOTOR AND NON-MOTOR SYMPTOMS |
| Drooling due to slowed swallowing (Sialorrhea) |
| Speech and swallowing problem |
Putting Your
Comprehensive Care Team
Together

Patients suffering from complex, chronic illnesses, such as PD,
benefit most from an interdisciplinary team of professionals
collaborating to provide individualized treatment and a care
plan designed to enhance the quality of life. The National
Parkinson Foundation (NPF) promotes this approach in our
Centers of Excellence and
Care Consortium networks.
Members of a comprehensive care team
Neurologists are doctors who specialize in
problems with the nervous system. A movement disorders
specialist is a neurologist who has completed an extra
one-to-two years of training in movement disorders such as PD.
The neurologist will monitor your case of PD, work with you to
prescribe appropriate medications, monitor your response to
therapies and make recommendations for care.
Primary Care Providers (PCP) are usually the
first point of contact and are usually internists or family
practice physicians who will manage your overall health. Don’t
be afraid to ask the family doctor for a referral to a
specialist. Your PCP should receive periodic reports from your
neurologist regarding the current management of your PD.
Physician’s Assistants (PA) have an advanced
degree and work under the supervision of a physician.
Nurses are often your primary contact and
the central coordinator of your care. Nurse Practitioners (NP)
are Registered Nurses (RN) who have an advanced degree and who
have passed special licensing requirements. Nurse Practitioners
can perform physical exams and prescribe medications and other
therapies. They often work with a physician, although they can
function independently.
Social Workers provide non-medical
assistance and work in a variety of hospital and community
settings. Many provide individual, couple and family counseling
to help persons cope with stressful life events. Social workers
often lead support groups. They can also help you to connect
with a variety of community resources and help you and your
family plan for the future.
Physical Therapists (PT) are licensed
professionals who evaluate and treat mobility problems such as
flexibility, strength, balance, posture and walking. They design
exercises or provide training to meet an individual’s needs. A
PT can also help family caregivers by teaching safe and
effective ways to provide assistance.
Occupational Therapists (OT) help to modify
or adapt activities of daily living which include dressing,
feeding oneself, getting in and out of bed, writing, and
performing in the workplace. An OT can address issues of safety
and independence in the home.
Speech-Language Pathologists (S-LP) are
health care professionals trained to assess, manage and treat
speech, voice, memory and swallowing problems. Treatment with a
therapist can improve problems you may experience with
communication or eating.
Nutritionists/Dieticians can help you design
an eating plan for overall health. A Nutritionist can be
particularly helpful if you have trouble chewing or swallowing,
difficulty preparing nutritious meals or problems with your
weight.
Pharmacists provide valuable information
about prescription medication and can provide counsel on
possible drug interactions and side effects. Try to use the same
pharmacy all the time so there is a record of all medications
being taken.
Neuropsychologists are licensed
psychologists with expertise in how behavior and cognitive
(thinking) skills are related to brain structure and symptoms.
Psychiatrists are physicians who specialize
in the diagnosis and treatment of mental, behavioral or
emotional problems such a
depression
and anxiety.
These symptoms may require specialized treatment.
Psychologists can work with individuals and
family members by providing advice and counseling for coping
with the disease.
Please also remember, that your caregivers and loved ones
are often your best advocates and can help you communicate with
your health care team.
Want to Learn More?
Print this checklist:
Building a Support Network
Print this checklist:
Making the Most of Your Medical Appointment
Read this "Parkinson Report" article:
Assembling a Comprehensive Care Team
Read this "Parkinson Report" article:
Social Workers in the Forefront
Watch this video:
What are some strategies to improve the quality of community
care for PD patients?
Watch this video:
Why is comprehensive care or a team approach important?
Medical content reviewed by: Nina Browner, MD—Medical
Director of the NPF Center of Excellence at the University of
North Carolina at Chapel Hill in North Carolina and by Fernando
Pagan, MD—Medical Director of the NPF Center of Excellence at
Georgetown University Hospital in Washington, D.C.
10 Early Warning Signs
of Parkinson's
Disease
Sometimes it is hard to tell that you might have
Parkinson's
disease. Parkinson's disease is when your brain stops
making an important chemical called
dopamine.
This chemical helps your body to move, and helps your mood. If
you do have Parkinson's, you can feel better by taking a pill
that helps your body to replace that chemical. Parkinson's
disease will get worse slowly over time, and your doctor can
help you stay healthy longer. Some of the problems listed here
could be signs of Parkinson's disease.
No single one of these signs means that you should worry
about Parkinson's disease. If you have more than one symptom,
you should make an appointment to talk to your doctor.
Early diagnosis of Parkinson's disease gives you the best
chance of a longer, healthier life.
What you can do if you do have Parkinson's disease:
- Work with your doctor to create a
plan to stay healthy. This plan might include:
- A referral to a neurologist, a doctor who specializes in
the brain
- Care from an occupational therapist, physical therapist
or speech therapist
- Meeting with a medical social worker to talk about how
Parkinson's will affect your life
- Start a regular exercise program to delay further
symptoms.
- Talk with family and friends who can provide you with the
support you need.
 Tremor
or Shaking Tremor
or Shaking
Have you noticed a slight shaking or
tremor
in your finger, thumb, hand, chin or lip? Does your leg shake
when you sit down or relax? Twitching or shaking of limbs is a
common early sign of Parkinson’s disease.
What is normal?
Shaking can be normal after lots of exercise, if you have been
injured, or could be caused by a medicine you take.
 Small
Handwriting Small
Handwriting
Has your handwriting suddenly gotten much smaller than in it
was in the past? You may notice the way you write words on a
page has changed, such as letter sizes are smaller and the words
are crowded together. A sudden change in handwriting is often a
sign of Parkinson’s disease.
What is normal?
Sometimes writing can change as you get older, if you have stiff
hands or fingers or poor vision, but this happens over time and
not suddenly.
 Loss of
Smell Loss of
Smell
Have you noticed you no longer smell certain foods very well?
If you seem to have more trouble smelling foods like bananas,
dill pickles or licorice, you should ask your doctor about
Parkinson’s disease.
What is normal?
Your sense of smell can be changed by a cold, flu or a
stuffy nose, but it should come back after you are better.
 Trouble
Sleeping Trouble
Sleeping
Do you thrash around in bed or kick and punch while you are
deeply asleep? You might notice that you started falling out of
bed while asleep. Sometimes, your spouse will notice, or will
want to move to another bed. Sudden movements during sleep may
be a sign of Parkinson’s disease.
What is normal?
It is normal for everyone to have a night when they ‘toss and
turn’ instead of sleeping.
 Trouble
Moving or Walking Trouble
Moving or Walking
Do you feel stiff in your body, arms or legs? Sometimes
stiffness goes away as you move. If it does not, it can be a
sign of Parkinson’s disease. You might notice that your arms
don’t swing when you walk, or maybe other people have said you
look stiff. An early sign might be stiffness or pain in your
shoulder or hips. People sometimes say their feet seem ‘stuck to
the floor.’
What is normal?
If you have injured your arm or shoulder, you may not be able to
use it as well until it is healed or another illness like
arthritis might cause the same symptom.
 Constipation Constipation
Do you have trouble moving your bowels without straining
every day? Straining to move your bowels can be an early sign of
Parkinson’s disease and you should talk to your doctor.
What is normal?
If you do not have enough water or fiber in your body, it can
cause problems in the bathroom. Also some medicine will cause
constipation too. If there is no other reason such as diet or
medicine that would cause you to have trouble moving your
bowels, you should speak with your doctor.
 A Soft or
Low Voice A Soft or
Low Voice
Have other people told you that your voice is very soft when
you speak in a normal tone, or that you sound hoarse? If there
has been a change in your voice you should see your doctor about
whether it could be Parkinson’s disease. Sometimes you might
think other people are losing their hearing, when really you are
speaking more softly.
What is normal?
A chest cold or other virus can cause your voice to sound
different but you should go back to sounding the same when you
get over your cough or cold.
 Masked
Face Masked
Face
Have you been told that you have a serious, depressed or mad
look on your face more often, even when you are not in a bad
mood? This serious looking face is called masking. Also, if you
or other people notice that you have a blank stare or do not
blink your eyes very often, you should ask your doctor about
Parkinson’s disease.
What is normal?
Some medicines can cause you to have the same type of
serious or staring look, but you would go back to the way you
were after you stopped the medication.
 Dizziness
or Fainting Dizziness
or Fainting
Do you notice that you often feel dizzy when you stand up out
of a chair? Feeling dizzy or fainting can be signs of low blood
pressure and can be linked to Parkinson’s disease.
What is normal?
Everyone has had a time when they stood up and felt dizzy, but
if it happens on a regular basis you should see your doctor.
 Stooping
or Hunching Over Stooping
or Hunching Over
Are you not standing up as straight as you used to? If you or
your family or friends notice that you seem to be stooping,
leaning or slouching when you stand, it could be a sign of
Parkinson’s disease.
What is normal?
If you have pain from an injury or if you are sick, it might
cause you to stand crookedly. Also, a problem with your bones
can make you hunch over.
Made possible through the generous support of the
Medtronic Foundation and thousands of people with Parkinson's
and their families.
|






 Parkinson’s
disease (PD) is a
Parkinson’s
disease (PD) is a

 Tremor
or Shaking
Tremor
or Shaking Small
Handwriting
Small
Handwriting Loss of
Smell
Loss of
Smell Trouble
Sleeping
Trouble
Sleeping Trouble
Moving or Walking
Trouble
Moving or Walking Constipation
Constipation A Soft or
Low Voice
A Soft or
Low Voice Masked
Face
Masked
Face Dizziness
or Fainting
Dizziness
or Fainting Stooping
or Hunching Over
Stooping
or Hunching Over




